Survey of 118 registered nurse managers finds strong conditional readiness for AI, but adoption depends on RN control, auditability, workflow fit, and measurable reduction in duplicate charting in Black Book Nursing Week 2026 series
CHICAGO, May 7, 2026 (Newswire.com)
–
In recognition of Nurses Week 2026, Black Book Research today released a new special report, “The Nurse Documentation and AI Readiness Gap,” finding that registered nurses are open to artificial intelligence documentation support, but only if the technology reduces redundant charting, preserves nurse control, and does not shift legal or audit risk to bedside clinicians.
The vendor-agnostic report is based on a survey of 118 registered nurse managers conducted between January and April 2026. Respondents represented nurse manager, assistant nurse manager, charge nurse, nursing informatics, quality, care coordination, case management, and comparable nursing leadership roles across hospitals, health systems, ambulatory, post-acute, and specialty care settings.
Black Book found that documentation burden is no longer viewed by nurse leaders as a simple electronic health record usability issue. Instead, nurse managers describe it as a direct-care displacement problem that affects bedside time, patient education, discharge preparation, family communication, coaching of newer nurses, and staff retention.
Among the key findings:
-
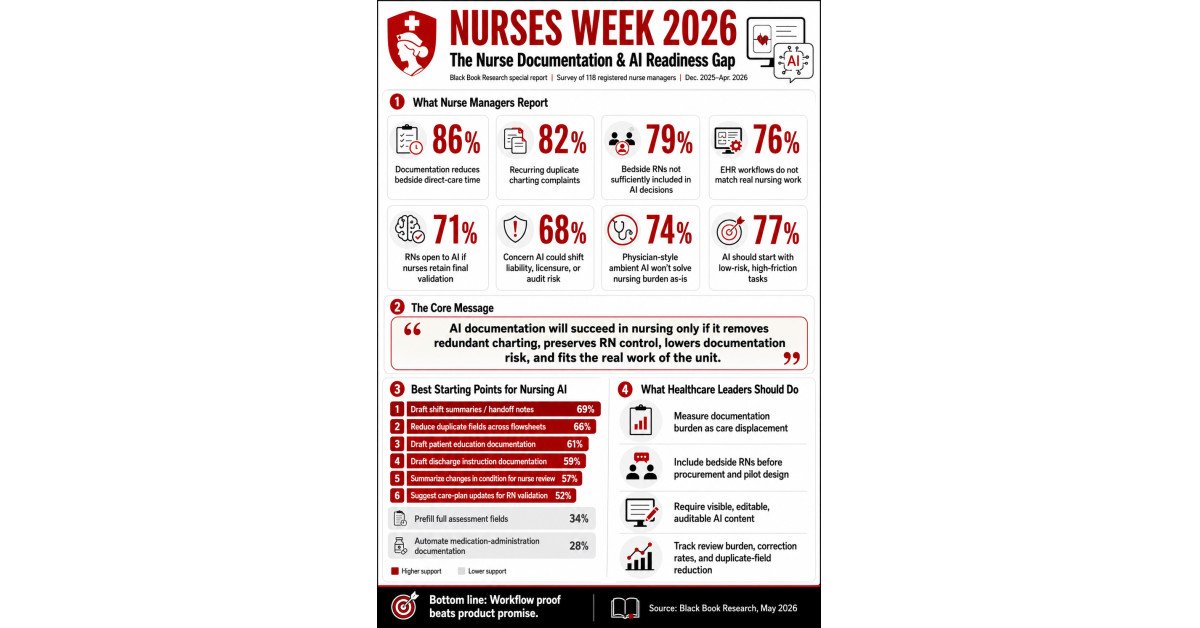
86% of nurse managers report that documentation requirements regularly reduce staff RN time available for direct patient care.
-
82% report recurring staff RN complaints about duplicate or overlapping documentation.
-
79% say bedside RNs are not sufficiently included in AI documentation design, vendor selection, pilot testing, governance, or rollout decisions.
-
71% believe staff RNs would use AI documentation support if nurses remain the final validators and AI-generated content is visible, editable, and auditable.
-
68% worry AI-generated or prefilled documentation could shift legal, licensure, audit, or patient-safety risk to nurses without meaningfully reducing workload.
-
74% say physician-style ambient documentation tools will not solve nursing documentation burden unless redesigned for nursing-specific workflows.
-
77% prefer AI documentation tools begin with low-risk, high-volume tasks before moving into autonomous assessment or clinical judgment support.
“These registered nurses are not asking technology to document more. They are asking technology to remove redundant work, protect professional judgment, and return time to patients,” said Doug Brown, Founder of Black Book Research. “The test for nursing AI is not whether it can generate a convincing note. The test is whether nurse managers and bedside RNs can prove it makes unit work safer, faster, clearer, and less documentation-heavy under real patient-care conditions.”
The report cautions that AI documentation tools designed primarily around physician encounter notes, billing capture, or executive demonstrations may fail in nursing environments.
Nursing documentation is shift-based, structured, multi-patient, longitudinal, and interruption-driven. It includes assessments, medication administration, reassessments, education, care plans, discharge readiness, risk screens, handoffs, escalation documentation, and patient responses across an entire shift.
Black Book identifies duplicate charting as the clearest near-term target for AI-enabled documentation relief. Nurse managers cited repeated flowsheet fields, quality and regulatory screens, care-plan documentation, patient education fields, discharge readiness documentation, and risk-screening silos as major sources of recurring RN frustration.
The report recommends that hospitals and health systems treat nursing AI documentation as a practice redesign initiative rather than a technology implementation. Before procurement or rollout, Black Book advises provider organizations to establish bedside RN governance, baseline documentation burden, separate use cases by risk level, prohibit silent prefill of high-liability fields, and measure post-go-live review burden, correction rates, duplicate-field reduction, after-shift charting, and documentation overtime.
For EHR and AI documentation vendors, the report’s message is direct: nursing AI is a distinct product problem. The winning tools will not be those that generate the most documentation, but those that remove the most redundant documentation while preserving RN control, transparency, source visibility, editability, and auditability.
“Workflow proof beats product promise,” Brown said. “Hospitals should not claim nursing AI readiness until bedside RNs can demonstrate that the tool reduces redundant charting, preserves professional judgment, lowers review burden, and fits the real work of the unit.”
About the Report
“The Nurse Documentation and AI Readiness Gap” is a Black Book Research Nurses Week 2026 special report examining documentation burden, EHR workflow design, AI readiness, liability concerns, governance gaps, and nursing-specific AI documentation use cases. The report is intended for nurse executives, health system leaders, EHR vendors, AI documentation companies, quality leaders, compliance teams, legal stakeholders, payers, and policy leaders. Industry stakeholders and media may download the report directly from the Black Book Research website or email the Press Office to request.
About Black Book Research
Black Book Research provides independent, vendor-agnostic healthcare technology, services, and market research. Black Book’s healthcare surveys and advisory reports support decision-making across hospitals, health systems, physician organizations, payers, technology vendors, and policy stakeholders globally.
Media Contact:
Black Book Research
research@blackbookmarketresearch.com
blackbookmarketresearch.com
SOURCE: Black Book Research
Source: Black Book Research