For the first time since 2018, the American College of Cardiology and the American Heart Association have released updated clinical guidance on how to screen for and manage blood cholesterol. The recommendations were published in the Journal of the American College of Cardiology and Circulation and were presented March 28 at the American College of Cardiology’s 75th Annual Scientific Session in New Orleans.
The release comes shortly before a related paper, “The ABCs of Cardiovascular Disease Prevention: Communicating What We Know in 2026,” appeared in the American Journal of Preventive Cardiology.
Focus on LDL, Lipids, and Personalized Risk
The updated guidance centers on lowering low-density lipoprotein (LDL) cholesterol, commonly known as bad cholesterol, along with other blood fats such as lipoprotein(a), or Lp(a). It also highlights the need for earlier screening, particularly for people with a family history of heart disease, and calls for more individualized risk assessments based on factors like existing health conditions. These steps are intended to support more informed, shared decisions between patients and clinicians.
“We know that lower LDL cholesterol levels are better when it comes to reducing the risk of heart attacks, strokes and congestive heart failure,” says Roger S. Blumenthal, M.D., chair of the guideline writing committee and director of the Johns Hopkins Ciccarone Center for the Prevention of Cardiovascular Disease. “We also know that bringing elevated lipids and blood pressure down in young adults supports optimal heart and vascular health throughout a person’s life.”
Why Earlier Screening Matters
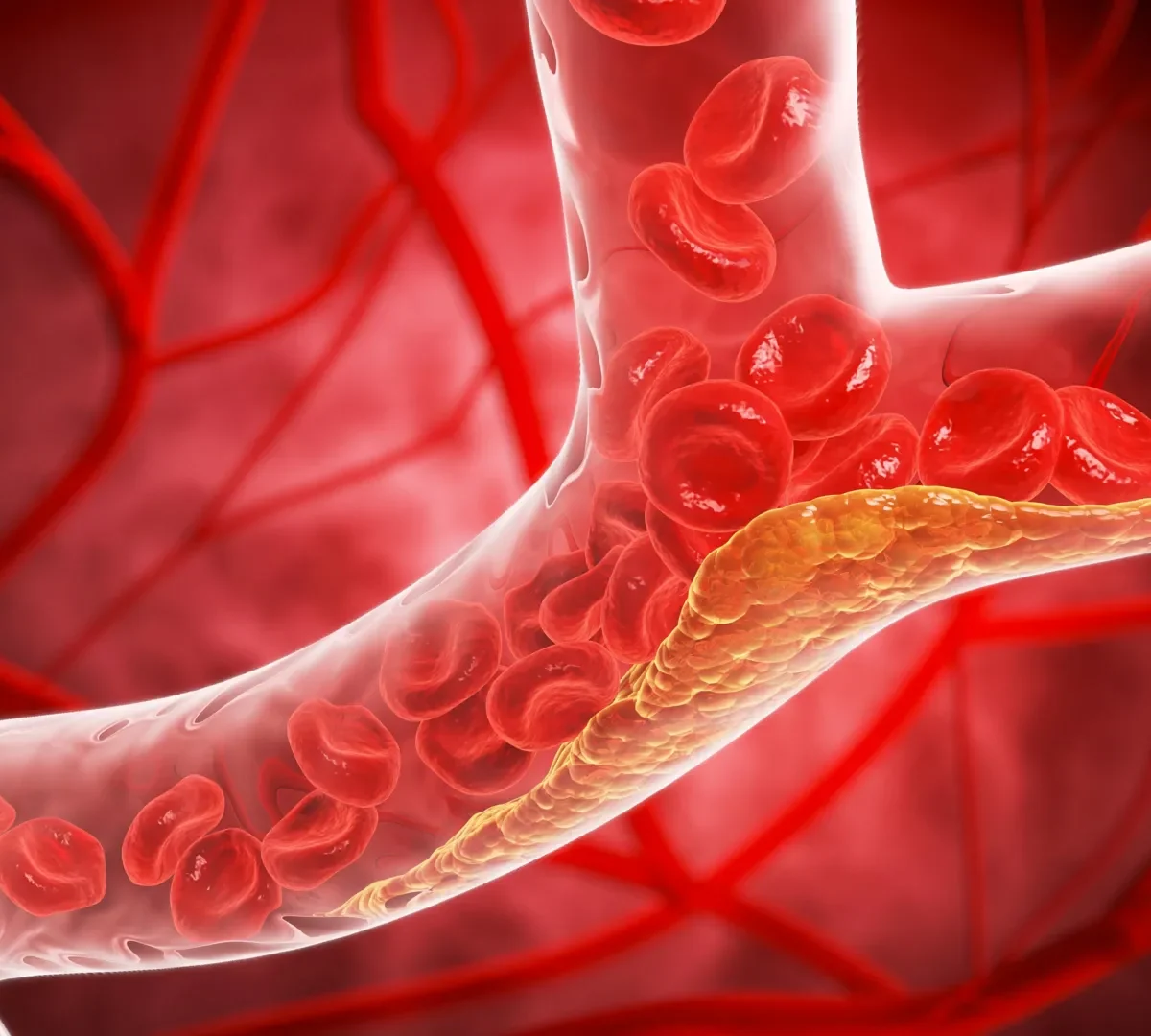
The update arrives as research shows that about 1 in 4 adults in the United States has elevated LDL cholesterol (LDL-C), a major contributor to atherosclerosis (the narrowing or hardening of the arteries). When certain lipids build up, they can form plaque inside artery walls. This plaque can restrict blood flow, and under certain conditions, it may rupture and trigger a heart attack or stroke or require urgent medical treatment to restore circulation.
Despite these risks, the core advice for maintaining heart health remains unchanged. Experts continue to stress the importance of a balanced diet, regular physical activity, avoiding tobacco, getting enough sleep, and maintaining a healthy weight. According to Blumenthal, roughly 80% to 90% of cardiovascular disease is linked, at least in part, to factors people can modify, making lifestyle changes a critical first step.
Earlier Screening and Genetic Risk Factors
A key shift in the new guideline is the push for screening at younger ages and a broader look at personal risk. Doctors are encouraged to consider family history of atherosclerosis, underlying conditions such as rheumatoid arthritis, and life events like early menopause or pregnancy complications, including preeclampsia or gestational diabetes, when evaluating risk and planning treatment.
For instance, individuals with familial hypercholesterolemia, a genetic condition that causes very high LDL-C levels, should now begin screening earlier in life, starting around age 9 (or earlier). The guidance also recommends a one-time test for Lp(a), which is tied to inherited risk and can raise heart disease risk by about 40% at levels of 125 nanomoles per liter and double the risk at 250 nanomoles per liter.
New Risk Calculator Expands Long-Term Prediction
Another major update is the introduction of a new tool for estimating 10- and 30-year risk of heart attack and stroke. The previous model focused mainly on 10-year risk for adults age 40 and older and relied on basic factors such as age, cholesterol levels, and blood pressure.
The new calculator, Predicting Risk of Cardiovascular Disease EVENTs (PREVENT), includes additional measures such as blood sugar and kidney function. It is designed for use starting at age 30 and is based on data from 6.6 million people, compared to just 26,000 in the earlier model.
“Shifting the paradigm toward proactive prevention strategies earlier in life can meaningfully change the trajectory of cardiovascular disease and lead to better health outcomes for people decades later,” says Seth Martin, M.D., M.H.S., a cardiologist and member of the guideline writing committee.
Additional Tests and Personalized Treatment Decisions
To further refine risk estimates, the guideline outlines additional factors doctors may consider, referred to as “risk enhancers.” For people with borderline or moderate risk, clinicians may use extra tests to guide decisions. These can include measuring inflammation through high-sensitivity C-reactive protein (hsCRP), evaluating Lp(a) levels, and reviewing family history and ancestry.
Imaging tools such as coronary artery calcium scans are also recommended to detect calcium deposits that signal plaque buildup, helping tailor treatment plans more precisely.
Expanded Treatment Options and Lower LDL Targets
The updated guidance addresses treatment strategies for a wide range of groups, including pregnant or breastfeeding individuals, adults age 75 and older, and people with conditions such as diabetes, advanced kidney disease, HIV, or cancer.
In addition to statins, the guideline includes updated recommendations on other cholesterol-lowering therapies, including ezetimibe, bempedoic acid, and injectable PCSK9 monoclonal antibodies. These options are particularly important for individuals who do not respond well to statins or require multiple therapies to reduce LDL-C.
For people without cardiovascular disease, LDL-C levels below 100 mg/dL are considered optimal. Those at intermediate risk are advised to lower levels below 70 mg/dL, while high-risk individuals should aim for less than 55 mg/dL. The guideline also includes targets for non-HDL cholesterol and apolipoprotein B.
Looking Ahead
In an accompanying editorial, experts suggest that future recommendations may further emphasize lowering LDL-C to below 55 mg/dL for people with moderate atherosclerosis. This direction is supported by findings from the VESALIUS-CV clinical trial, which showed benefits from aggressively lowering cholesterol using a combination of therapies.
The 2026 Guideline on the Management of Dyslipidemia was developed by the American College of Cardiology and the American Heart Association in collaboration with multiple medical organizations focused on cardiovascular health, prevention, and patient care.